Introduction: Why AI in Liver Care Marks a New Evolution
What does it mean to be human in a world evolving from muscle-driven labour, through an age of intellect, into today’s era of AI-powered medicine? For centuries, survival depended on strength; with machines, knowledge, and creativity took precedence. Now, with AI redefining liver care, we face the next great leap towards fast, fair, preventive, and personal healthcare.
This blog will take you from the roots of human evolution, through the muscle-to-mind transition, into the age of AI in liver care, and into a bold, utopian future. You’ll find evidence, quotes from real studies, and a unique voice on using AI in liver care for personal transformation, prevention, and better living.
The Journey: From Muscle to Mind to AI in Liver Care
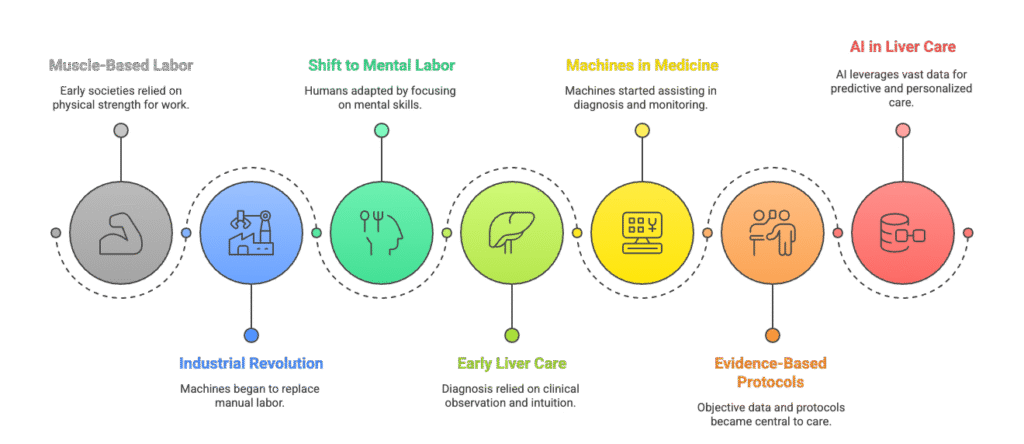
Historical Perspective: From Muscle to Mind to Machines
Before the Industrial Revolution (roughly late 18th to early 19th century), strength, endurance, and manual skill were central to survival and social value. Machines amplified human capacity, but also displaced certain types of work. That was a huge societal and psychological shift: people feared being “made irrelevant” by machines. Over time, humans adapted, and they began emphasising creativity and problem-solving, areas where machines couldn’t fully replace them.
In the early days, diagnosis did not rely on sophisticated machines or laboratory reports. Clinical practice was centred around the art of history taking and meticulous physical examination. Diagnoses were often made based on subtle signs, careful observation, and intuition. There was no standardised evidence or protocols: the reputation of a clinician largely depended on their skill in clinical reasoning and bedside acumen.
The Gradual Shift: Machines and Evidence Take Centre Stage
As medicine advanced, machines began to assist with diagnosis and monitoring. Imaging, laboratory analysis, and standardised procedures transformed how disease was detected and treated. What was once based solely on clinical judgment gradually incorporated objective data and reproducible evidence. This transition marked a major shift; while the clinician’s insight remained vital, technology and evidence-based protocols now drive accuracy and consistency in modern health care.
Era of AI —Predictive, Personalised Wellness
The concept of artificial intelligence in medicine is far from new; the term “AI” was coined back in the 1950s. What sets today’s era of AI in health and liver care apart is the monumental scale and richness of data now available. Decades ago, our resources were limited, patient histories and examinations relied on clinical memory, word of mouth, and sparse written records. Now, with the explosion of digital technology, we have access to vast volumes of health information: laboratory data, genetic profiles, imaging, audio notes, even video and lifestyle metrics. AI in liver care learns not only from structured medical datasets, but from real-world inputs that reflect lived experience.
Modern AI in liver care is different because it leverages patterns across this immense data landscape. The more data it receives, clinical notes, scans, lab results, treatments, and outcomes, the smarter it becomes. AI in liver care ‘evolves’ each day with every new record, update, and integration. What makes AI truly remarkable is its capacity to find new correlations, detect hidden trends.
As AI in liver care continues to evolve, we may find it capable of solving clinical mysteries that have puzzled experts for generations, creating preventive strategies, and suggesting novel treatments that would have taken decades for traditional research to uncover.
Modern Era: Integrating Technology and Clinical Excellence
Today, the best liver clinicians seamlessly blend their deep experiential understanding of disease with the insights that come from laboratories, imaging suites, and increasingly, algorithms. Machines do not replace the doctor, but expand capacity, making quality care reproducible, scalable, and globally sharable.
While the backbone of liver medicine is still the artful clinician, the integration of technology enables rapid diagnosis, fosters earlier intervention, and supports more consistent practice across environments.
AI in Liver Care: Evidence-Based Advances and Where We Stand in 2025
The field of AI in liver care has witnessed a rapid transformation in recent years, moving from theoretical promise to practical, real-world clinical application. The integration of artificial intelligence into hepatology is fundamentally changing how liver diseases will be diagnosed and managed. AI can enable earlier detection, predict disease progression, and support more precise treatment strategies. Here’s where we stand:
- AI and machine learning have shown great promise in research settings for early risk prediction and aiding diagnosis in liver disease, particularly with imaging and large datasets. However, most tools remain in validation or pilot usage in leading centres, and their impact on routine global practice is still limited.
- Most AI models require substantial clinical data, careful validation, and often struggle with integration into everyday clinical workflows, especially outside major academic hospitals or research studies.
- While deep learning can match expert performance in some imaging tasks and decision support, it is not yet widely replacing human judgment, nor is it the standard of care everywhere.
- In transplantation, experimental AI models are being trialled for allocation and matching.
- Real-world adoption faces challenges related to regulatory, technical, data quality, and ethical/interpretability issues.
- AI is reshaping HCC management—detecting disease earlier, stratifying risk more precisely, and guiding therapy through individualised prediction. However, broad clinical adoption depends on rigorously validated, interpretable, and accessible models.
- AI holds significant promise for transforming liver transplantation—making care more precise and individualised in both pre- and post-transplant settings. However, robust translation into routine clinical workflows will require better data, prospective validation, and clear real-world evidence of benefit
- Metabolically-dysfunction-associated steatotic liver disease (MASLD) is rapidly becoming a major cause of chronic liver disease. Artificial intelligence (AI) has recently gained prominence in healthcare for its capabilities in diagnostics, patient care, and drug development, showing strong promise for its use in MASLD.
- Artificial intelligence and Machine learning show significant promise for managing cirrhosis and its complications, but wide clinical integration demands further validation and user-friendly workflows.
- Precision medicine represents a major shift from “one-size-fits-all” treatment to highly individualised care. Here, AI is indispensable in handling and interpreting huge and complex datasets—including patients’ genetic makeup, clinical history, lifestyle factors, and environmental exposures. AI-driven precision medicine is creating new standards for efficacy, safety, and patient experience.
- AI-Assisted Surgery guided by real-time data analysis and intelligent algorithms, surgical robots can execute precise, minimally invasive procedures with unprecedented dexterity and control. AI can help avoid complications, reduce errors, anticipate anatomical variations, and adapt strategies during the procedure. This leads to shorter recovery times, less scarring, and better surgical outcomes.
These advancements, supported by robust data, evolving technology, and human expertise, are driving healthcare into an exciting future, where diagnosis, treatment, and patient care are more effective, compassionate, and individualised than ever before.AI in liver care is advancing rapidly in research and some specialist settings. The promise is huge, but outside of a few elite centres, most liver clinicians in 2025 are still relying on established methods. AI is an evolving assistive tool, not a universal clinical reality yet.
Utopian Medicine and AI
Based on current thinking in futurism, neuroscience, and philosophy, the next “human frontier” may not be muscle or mind in the traditional sense. Some ideas include:
- Emotional Intelligence & Social Connection
AI can analyse data and perform tasks, but genuine empathy, intuition, and emotional creativity are still uniquely human. Relationships, mentorship, leadership, and emotional resonance might become even more valuable in the future. - Consciousness & Self-Awareness
Understanding one’s own mind, ethics, morality, and the deeper questions may become the core domain of human endeavour. - Creativity Beyond Algorithmic Prediction
AI can generate music, art, and writing, but original, disruptive creativity that breaks patterns may still rely on humans. Innovation might shift from manual or analytic execution to “conceptual imagination”, seeing things that have never been thought of. - Curiosity & Exploration
Humans may focus on exploration of the physical and metaphysical universe, space, quantum realities, or dimensions of consciousness. Curiosity-driven discovery could be a core human role. - Integration of Technology & Biology
The next era could involve humans merging with machines, bio-augmentation, neural interfaces, and memory enhancement. The boundary between AI and human intelligence may blur. The “next thing” may be enhancing the human experience itself, rather than competing with AI.
In short, the next thing could be the uniquely human experience, our emotional, ethical, and creative capacities.
AI in Liver Care: Challenges and Ethics
1. Data Complexity
AI thrives on massive, diverse, and accurate datasets—clinical records, labs, imaging, pathology, and real-world outcomes. In various health care setups, data can be fragmented, incomplete, or inconsistent. Many clinics lack standardised electronic records or high-quality imaging archives, limiting AI’s learning and reliability. Without representative data, models may struggle to generalise, potentially missing rare presentations or regional differences in disease.
2. Clinical Integration
Most AI tools for liver care remain confined to pilot studies, research labs, or select academic hospitals. Full-scale integration into daily hospital workflows requires robust IT infrastructure, seamless interoperability with existing systems, and ongoing software support. Beyond technology, successful adoption depends on training clinicians and staff not just to use AI tools, but to interpret and trust their outputs appropriately.
3. Trust and Transparency
For AI to be accepted, clinicians and patients need to understand how models work and why recommendations are made. Ethical guidelines must address issues like patient consent, rights to explanation, risks of automation error, and liability. Transparent reporting and independent oversight build confidence and ensure accountable use.
4. Bias and Equity
AI models risk perpetuating and magnifying existing healthcare biases if not carefully designed and monitored. For AI in liver care, this means continually testing and refining algorithms to ensure fair, accurate performance for all populations: different ages, genders, ethnic backgrounds, and socioeconomic groups.
Successfully harnessing AI’s power in liver care requires more than technical innovation—it demands honest confronting of data limitations, systemic investment in integration, unwavering commitment to fairness, and rigorous validation. Only with this foundation can AI deliver its promise: safer, smarter, and truly equitable liver healthcare for the future
The Human-AI Partnership: AI in Liver Care and the Essence of Medical Progress
“AI in liver care augments human expertise, empowering clinicians rather than replacing them.”
Rather than an “AI versus humans” future, the reality is one of creative synergy. With AI handling the computational burden, clinicians can devote their energy to high-level reasoning, emotional support, advocacy, and lifelong learning.
Creativity, Reflection, Connection
- Creativity: AI provides clinicians with fresh insights and innovative approaches, inspiring new diagnostic strategies, treatment plans, and research directions.
- Reflection: Continuous feedback from AI-driven outcomes encourages clinicians to reflect, adapt, and improve their practice.
- Connection: AI can enhance communication among care teams and connect patients with tailored resources, facilitating truly collaborative, patient-centred care.
The essence of medical progress is found not in technology alone, but in the powerful partnership between people and AI. In liver care, this partnership is already transforming practice not by replacing, but by extending and enriching the art and science of medicine. The future will be shaped by those who combine the best of both worlds: human wisdom and empathy, augmented by intelligent, ethical technology.
AI in Liver Care: The Future—A 2030+ Roadmap
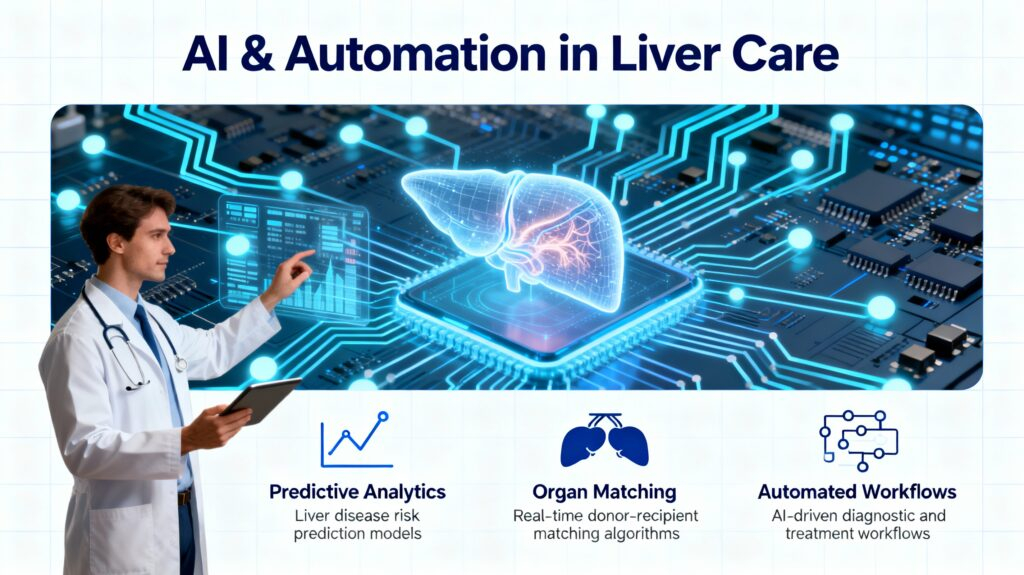
Automated Imaging Analysis in Daily Practice
- By 2030, AI-powered imaging will be routine, not cutting-edge. From ultrasounds to MRIs and CTs, algorithms rapidly and reliably identify early liver changes, flag suspicious lesions, and even suggest likely etiologies, minimising oversight and speeding up workflow. Radiologists will spend less time combing through negative scans and more time on consultations and nuanced cases.
- Sophisticated ML models will be embedded in electronic health records at tertiary centres, stratifying patients by individualised risk for cirrhosis, HCC, or decompensation in real-time. These predictions, constantly refined by new data, will guide schedules for monitoring, prompt earlier referrals for transplantation, and personalise treatments based on genetics, comorbidities, and even lifestyle data.
Dynamic Post-Transplant Care Models
- AI will help optimise immunosuppressive regimens and monitor for rejection or complications by integrating lab trends, drug levels, sensor data, and even patient-reported symptoms. Dynamic risk dashboards will predict who needs closer follow-up, allowing graft-saving interventions before problems become critical.
Improved Liver Cancer Screening, Earlier Intervention, Fewer Unnecessary Biopsies
- Screening programs will use AI to minimise false positives, prioritise soonest interventions for those most likely to benefit, and more accurately predict challenging features like microvascular invasion. Precision AI will help confidently rule out disease, too, so fewer healthy patients undergo unnecessary, invasive tests.
The Essence:
By 2030 and beyond, AI will not simply be about better algorithms, but better, more human-centred liver care faster, fairer, and more predictive. With AI as co-pilot, clinicians and health systems become more preventive, more connected, and far more responsive to individual needs and global threats alike.
Frequently Asked Questions
Q: Will AI in liver care replace doctors?
A: No, AI in liver care assists doctors in diagnosis and in precision in overall medical management by the doctors.
Q: Is my data safe with AI in liver care?
A: Yes, modern systems use anonymisation and privacy-preserving technology to secure patient data.
Q: How soon will every hospital use AI in liver care?
Q: What’s the single biggest promise of AI in liver care?
A: Empowering everyone regardless of geography or income, with the best possible prevention, diagnosis, and support for lifelong liver wellness.
🔄 Update (2025): AI Industry Trends & Global Perspectives
Recent global discussions highlight two evolving themes in the AI landscape:
• Market Realism:
Leaders like Sundar Pichai caution that while AI is progressing rapidly, the industry also shows signs of hype. A future correction is possible, reminding us to stay balanced, thoughtful, and grounded as AI expands.
• Human-Centred Superintelligence:
Insights from Eric Schmidt and Fei-Fei Li emphasise that true superintelligence is still distant and will require major breakthroughs. They also highlight that the biggest gains will come to nations and organisations that invest in people, partnerships, and their own technological foundations — always with human dignity at the centre.
These global perspectives enrich the broader conversation on how AI will shape healthcare, including liver care.
Conclusion: AI in Liver Care as Humanity’s Greatest Leap
In the dazzling dance of human-AI partnership in liver care, each step blends the intuition and compassion of skilled clinicians with the limitless analytical power of AI. While technology performs rapid calculations, spots patterns, and processes vast streams of data, it’s the human touch that feels, interprets, and inspires hope. Together, we forge an alliance where innovation and empathy move in harmony—AI enables doctors to focus on personalised healing, patients gain agency to participate in their own wellness, and liver care evolves into a truly holistic, collaborative journey. This partnership is not a replacement, but a celebration: technology amplifies our best human qualities, and together we leap towards a utopian future in health.
AI in liver care is the culmination of humanity’s journey from muscle to mind to meaning. It promises not just efficiency and fairness but a fundamental change in how we view wellness, prevention, and what it means to be human. The transition to a utopian world where medicine is personalised, preventive, and universal begins now. When we align muscle, mind, and heart, AI in liver care becomes not our competitor, but the truest tool for “being” our best selves.
Share this post, comment your vision for a utopian future, and let’s build the era of “better being” together—with AI in liver care, anything is possible!
📘 More Help for Your Liver Health Journey
🆓 Free eBooks by Dr. Tanuja Mallik:
- Know Your Medicine – Understand key post-transplant medications
- Best Foods for Liver Health – What to eat (and avoid) for optimal liver care
💬 Got a liver issue or recovering from transplant?
Book a 1-on-1 Online Consultation for personalised recovery & guidance.
🔗 Access all resources here: linktr.ee/drtanujamallik
